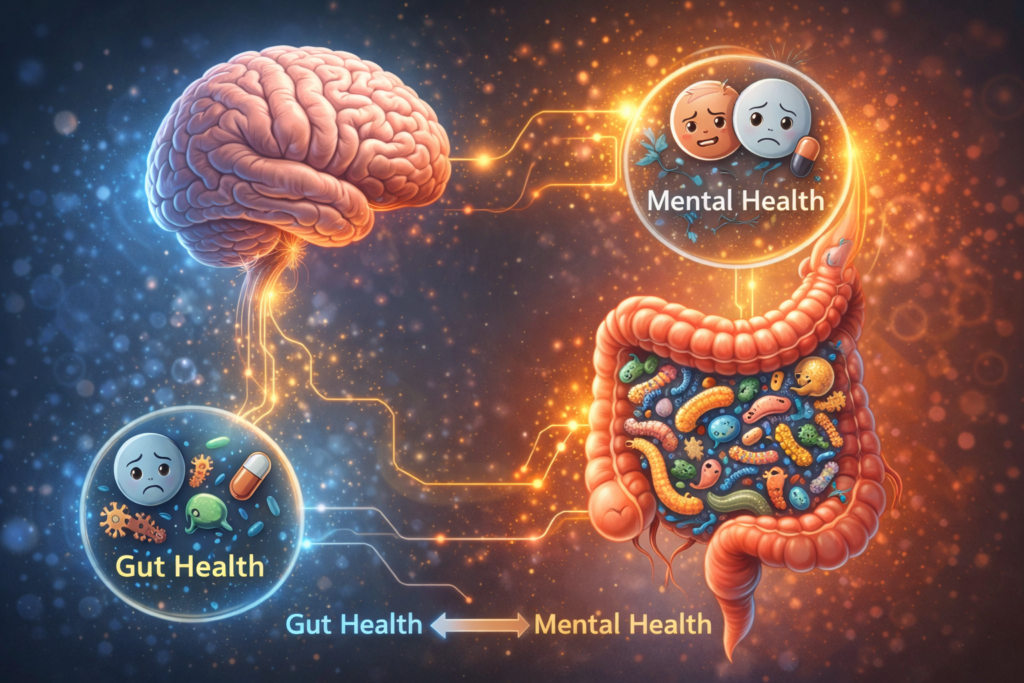
The gastrointestinal system and the central nervous system are functionally interconnected through what is commonly referred to as the gut–brain axis. This bidirectional communication network is mediated through neural, endocrine, immune, and metabolic pathways and represents a fundamental component of human physiology.
One of the clearest everyday examples of this connection is the body’s response to acute psychological stress. Situations such as public speaking, examinations, or emotionally charged events are frequently accompanied by gastrointestinal symptoms — nausea, abdominal discomfort, altered bowel movements, or a sudden loss of appetite. These responses occur in the absence of any structural gastrointestinal disease and are driven by neural and hormonal signaling between the brain and the gut.

This phenomenon illustrates the role of the enteric nervous system and its communication with the central nervous system, particularly via the vagus nerve. Stress-related activation of the autonomic nervous system alters gut motility and secretion almost immediately. At the same time, stress hormones influence intestinal barrier function and immune signaling, demonstrating how psychological states can directly modify gastrointestinal physiology.
The reverse relationship is equally familiar. Individuals experiencing prolonged digestive disturbances often report changes in mood, concentration, and stress tolerance. Chronic bloating, discomfort, or irregular bowel function can be associated with irritability, mental fatigue, and reduced emotional resilience. These experiences reflect the continuous signaling from the gut to the brain, mediated through inflammatory pathways, metabolic byproducts, and neuroactive compounds generated within the gastrointestinal environment.
The gut’s involvement in neurotransmitter-related processes further supports this link. Many of the biochemical precursors required for neural signaling are processed or regulated within the gut, and their availability can influence central nervous system function. While these processes are tightly regulated, disruptions in gut balance may alter signaling patterns that affect emotional and cognitive states.
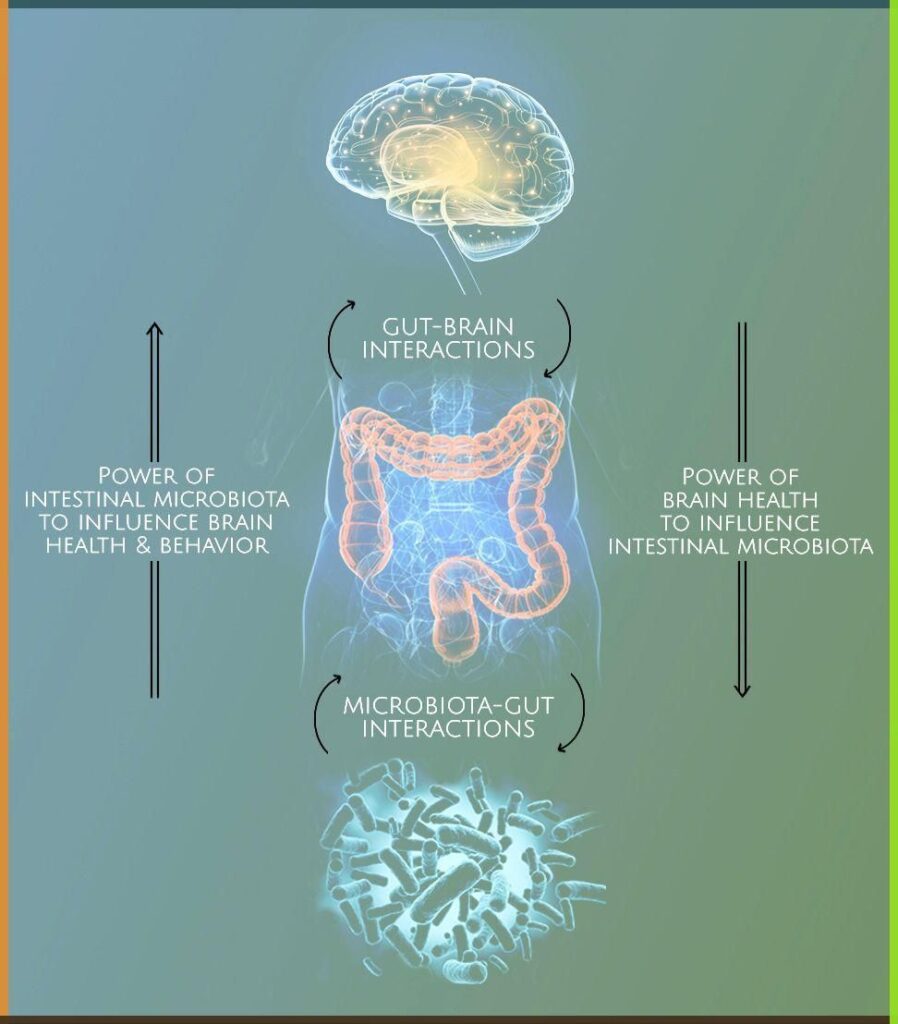
Stress physiology provides an additional layer of integration. Activation of the hypothalamic–pituitary–adrenal axis influences both brain and gut function simultaneously, reinforcing the concept that mental and gastrointestinal responses are coordinated rather than independent events.
Taken together, these observations demonstrate that the connection between gut health and mental health is not abstract or theoretical. It is experienced in everyday life and reflects normal biological communication within the body. Understanding this relationship encourages a more integrated view of mental health, grounded in systemic physiology rather than isolated organ function.
Lämna ett svar